Disclaimer:
This article is intended for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. We created this article in collaboration with Athena Aftercare, LLC ― an educational initiative on breast cancer aftercare with an immediate focus on helping survivors and caregivers learn about breast cancer-related lymphedema (BCRL).
BCRL is a complex medical condition, and you should make any management decisions in consultation with a qualified healthcare professional. While we base the information presented on current research and technological developments, individual patient needs may vary, and we do not guarantee outcomes.
The authors and 3DLOOK do not assume any liability for decisions made based on the content of this article. Always seek the guidance of your physician or other licensed healthcare provider with any questions regarding a medical condition or treatment.
Introduction: Why BCRL Deserves More Attention
Over the past three decades, advances in research and treatment have enabled an increase in the breast cancer survivorship rate by 40% in some high-income countries. Surviving breast cancer doesn’t mean a complete defeat of illness without any consequences, which makes long-term quality of life a central focus of breast cancer aftercare.
One of the most persistent and widespread challenges breast cancer survivors face is breast cancer-related lymphedema (BCRL), an incurable swelling of fluid in the arm, chest, breast and/or truncal area, which may develop months or years after treatment when the lymphatic system is damaged during surgery or radiation therapy. Although up to 65 % of women who undergo breast cancer surgery may suffer from lymphedema, and early intervention is crucial for better outcomes, BCRL is frequently underdiagnosed until visible swelling appears. Early lymphatic changes are subtle and easily overlooked or dismissed as temporary post-treatment effects during routine clinical exams.
«BCRL is difficult to diagnose at the critical onset period. One of the most frequently used screening tools is the circumferential tape measurement of a patient’s arms. The process is challenging for breast cancer survivors to do at home and can result in inaccurate measurements and recordkeeping.»
Lia Colabello, Founder of Athena Aftercare
There are several lymphedema diagnostic methods, including Bioimpedance Spectroscopy, Lymphoscintigraphy, and ICG Lymphography. These are expensive and must be done at a medical facility. Since BCRL must be tracked on a regular basis, this requires breast cancer survivors to visit medical care providers for their analog, and imprecise, tape measurement method.
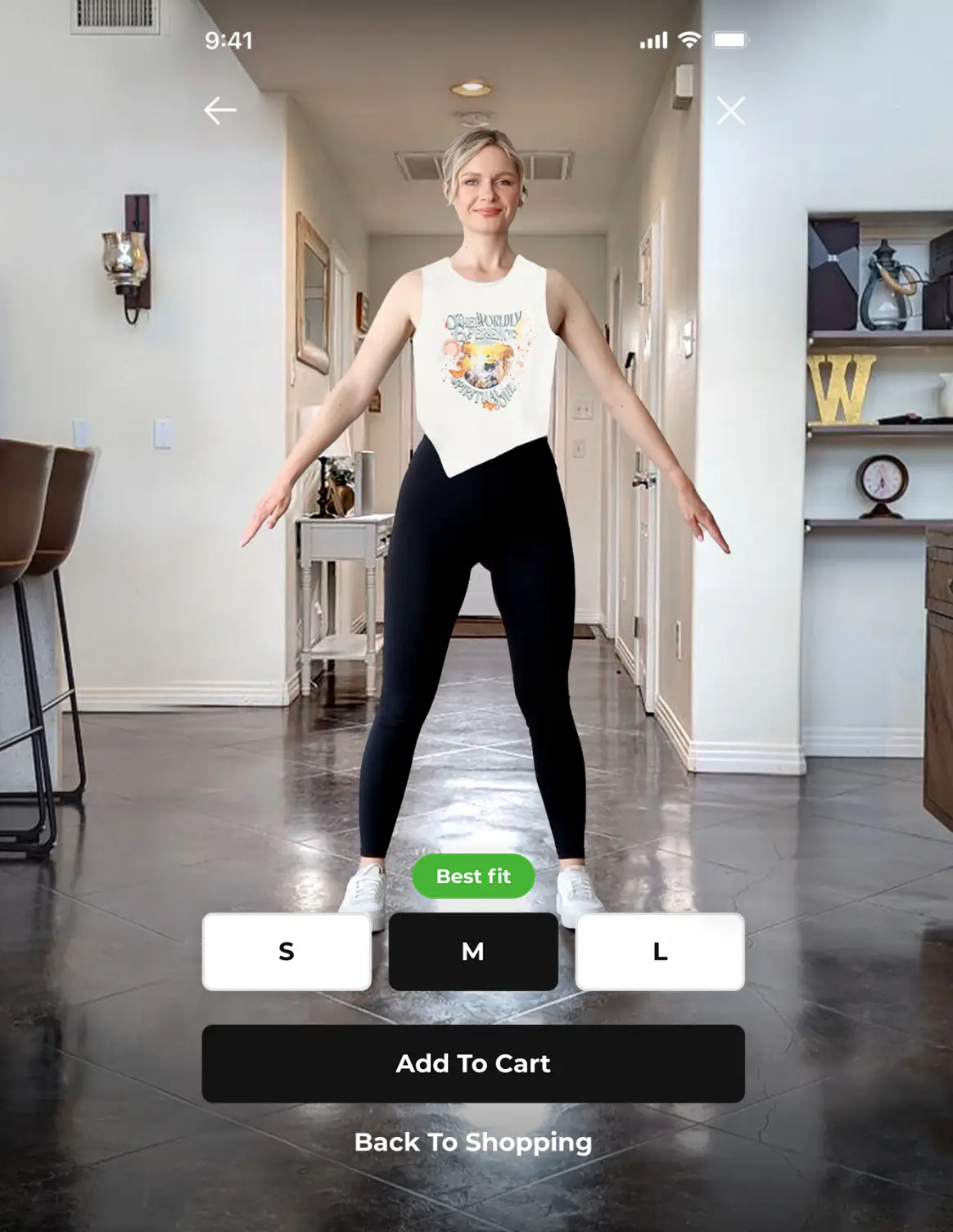
In response, an AI-powered 3D body-scanning solution based on smartphone-taken photos can be a cost-effective BCRL detection solution, enabling easily reproducible measurements of a patient’s body over time. Patients will be able to track their body measurements in the comfort of their own home, and contact their medical care provider to seek treatment if an anomaly is detected.
«Currently, we are conducting customer research to develop a solution that can digitally screen breast cancer survivors for BCRL with the help of 3DLOOK’s AI body measurement technology. If you are interested in participating in the study, click on this link.»
Lia Colabello, Founder of Athena Aftercare
What Is Breast Cancer-Related Lymphedema (BCRL)?
Definition of BCRL
Breast cancer-related lymphedema (BCRL) is a chronic condition resulting from swelling caused by the build-up of lymph fluid in surrounding tissues due to the blockage of impaired lymphatic drainage. BCRL is often a consequence of cancer treatment, and can occur decades after breast cancer surgery, so a survivor must be vigilant for this swelling for their entire lives.
How and Why BCRL Develops
Treatments that can lead to the disruption of normal lymph drainage and increase the risks of BCRL development include:
- Mastectomy. Removal of all or part of the breast damages the lymphatic vessels
- Lumpectomy. Lymph node removal limits drainage capacity
- Radiation therapy. Increases risk by inducing inflammation
- Scar tissue. Restrict lymph flow.
BCRL after radiation treatment is particularly challenging to detect. Swelling caused by radiation-related scar tissue development and gradual lymphatic impairment might be subtle and evolve slowly, making it problematic to distinguish from regular post-radiation changes. Therefore, the long-term monitoring of patients who received radiation therapy is critical.
Common Symptoms of Breast Cancer-Related Lymphedema and What Does It Look Like? (Visual Signs & Imaging)
Stages of Lymphedema
There are 4 stages of lymphedema:
| Stage | Symptoms | Considerations |
| 0 (latent or subclinical lymphedema) | No visible swelling (edema) or pitting, which refers to a temporary indentation in the skin when pressed. A mild tingling, slight heaviness, or tightness in the affected area | Develops months or years before obvious symptoms develop. |
| 1 (early or mild lymphedema) | Visible reversible swelling: a temporary small dent (or pit) forms when pressing the skin; no permanent damage to the skin or underlying tissues. | Once mild lymphedema develops, the risk for moderate lymphedema increases, even if the symptoms resolve with treatment. |
| 2 (moderate lymphedema) | Visible swelling with pitting. Inflammation, hardening, or thickening of the tissue under the skin that remains even if the affected area is elevated. | A higher risk of infection. Pitting may disappear after soft-tissue scarring. Tissue damage is irreversible. |
| 3 (severe lymphedema) | Visible swelling, the affected area enlarges and becomes misshapen. The skin hardens and thickens to the point that there is no pitting, and lymph can leak through damaged tissue. | The most advanced stage. Stage 3 lymphedema is relatively rare in people diagnosed with breast cancer. A high risk of infection |
BCRL can involve different anatomical regions, including the arm, hand, breast, chest and/or upper back on the side of the body affected by breast cancer surgery.
Arm and Upper-Body Symptoms

Arm swelling remains one of the most recognized manifestations of BCRL, and identifying these early arm and upper-body symptoms is essential:
- Beginning: mild, intermittent swelling accompanied by sensations of tightness, heaviness, or reduced mobility;
- Progression:
- visible arm swelling, changes in skin texture and difficulty wearing jewellery or clothing;
- pressure or fullness resembling clogged lymph nodes in the breast or underarm region;
- asymmetry and shape distortion.
Breast and Chest Symptoms

Lymphedema symptoms in the breast and chest area are easy to overlook or misattribute to treatment effects because they frequently develop gradually and may fluctuate.
Breast lymphedema symptoms:
- Breast swelling and heaviness;
- Increased tissue firmness and reduced elasticity in irradiated areas that alter the shape or feel of the breast;
- Pain or discomfort ranging from mild tenderness to persistent pressure.
While arm involvement in lymphedema is most widely recognized, breast or chest wall lymphedema requires broader evaluation strategies and is often diagnosed at a later stage.. Although initially resembling temporary inflammation, persistence or progression of breast edema after lumpectomy or radiation usually signals underlying lymphatic dysfunction. In some cases, changes in clothing or bra fit are noticed first.
Treatment Options for Breast Cancer-Related Lymphedema
There is no cure for lymphedema, but consistent therapy combined with monitoring technologies and supported by a patient’s knowledge and awareness of BCRL can reduce symptoms and significantly improve quality of life:
- Complete Decongestive Therapy (CDT) remains the foundation of BCRL management, encompassing manual techniques (including, but not limited to, manual lymph drainage), exercise, and skin care. These approaches aim to reduce swelling, maintain tissue health, and support lymphatic flow.
- Accurately fitting compression garments play a central role in daily management by controlling swelling and supporting lymphatic function. Medical alert bracelets complement compression by improving safety during emergencies and ensuring appropriate care.
- Athena Aftercare provides vital knowledge and resources to help breast cancer survivors manage this lifelong condition of BCRL.
Ideally, BCRL care management should begin as early as possible by working with a medical care provider to identify a nearby certified BCRL therapist trained in a CDT methodology like PORi or LANA. This specialist can help prevent BCRL from developing, determine if it occurs, and provide the necessary care if a patient develops symptoms. A certified BCRL therapist should be part of the care management team before and during cancer treatment, and track a breast cancer survivor’s aftercare progress for years.

Discover how AI-powered body intelligence is reshaping GLP-1 programs, telehealth, and digital health, from accurate remote assessments to safer and more engaging patient journeys.
Traditional Diagnosis and Monitoring: Where Care Falls Short
The earliest diagnosis of BCRL provides the best chance to reverse symptoms and prevent progression to more severe stages. Authoritative lymphedema-related medical societies, programs, and networks recommend preoperative assessment and ongoing surveillance of the ipsilateral and contralateral arms at regular, standardized intervals as best practice.
Conventional BCRL diagnosis relies on clinical examination and patient-reported symptoms, which are subjective and often address only visible or persistent swelling. It is easy to miss the early lymphatic changes, particularly when baseline measurements are unavailable.
Tape measurements focus on circumference at fixed points and are primarily designed for limbs, but are poorly suited to assessing diffuse breast or chest wall changes. The lack of standardized, breast-specific monitoring protocols reduces reproducibility and delays intervention, reinforcing a reactive care model.
How AI-Powered 3D Body Scanning Can Transform BCRL Detection, Monitoring, Care Management and Patient Engagement
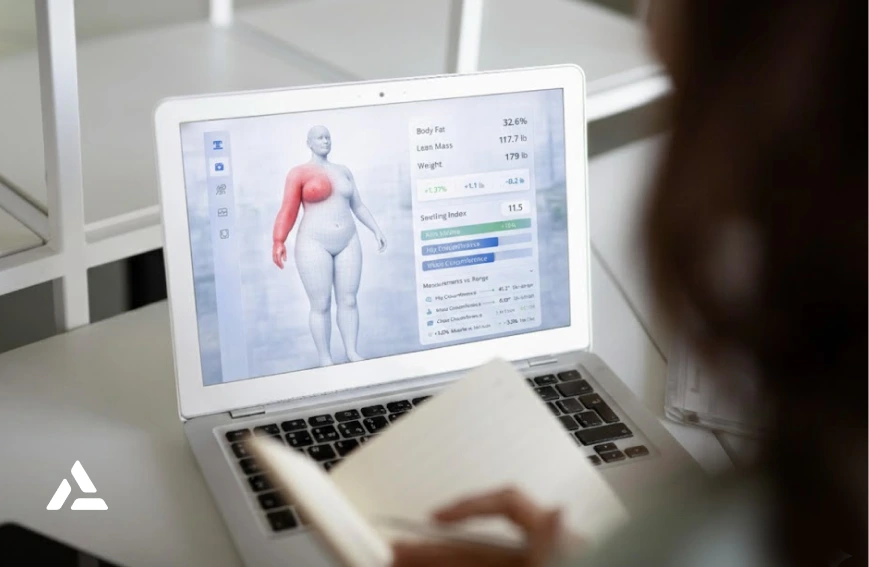
What Is AI-Powered 3D Body Scanning?
AI-powered 3D body scanning uses artificial intelligence to reconstruct a detailed three-dimensional body model from standard photographs. The process is non-contact and does not require specialized scanning equipment, enabling consistent, repeatable assessment without the need for physical measurement tools.
By capturing shape, volume, and asymmetry across the breast, chest wall, and arm, AI-driven reconstruction could provide anatomical detail beyond point-based circumference measurements. Each scan creates a digital record that can be stored and compared over time, supporting objective monitoring and data-informed clinical decisions.
Early Detection, Longitudinal Monitoring and Progress Tracking of Breast Cancer-Related Lymphedema
Athena Aftercare is working towards the day when photo-based 3D assessments will detect breast and arm lymphedema at a subclinical stage, before the visible swelling or patient-reported symptoms appear. Minor volumetric deviations and asymmetries, often undetectable through visual inspection or tape measurement, can be quantified with greater sensitivity.
Establishing an objective post-treatment baseline can enable accurate interpretation of future changes, as it accounts for individual anatomy and physiological asymmetry. Regular monitoring should allow for the detection of deviations from baseline and support timely, personalized interventions to reduce the likelihood of disease progression.
Repeated 3D assessments may enable evaluation of breast, chest wall, truncal, and/or arm volumes over time. This long-term recordkeeping could help distinguish expected post-treatment variability from early lymphatic dysfunction.
Role in Treatment Planning, Benefits for Patient Engagement and Care Teams
Trend analysis of the longitudinal monitoring data derived from AI-powered 3D body scanning can enable clinicians to adjust treatment plans before swelling becomes clinically significant. Quantitative volumetric data derived from AI-powered 3D models can support proper compression garment selection by accounting for complex anatomical contours in under 3 minutes, while the medical compression garment fitting procedure conducted by a certified fitter lasts 20-30 minutes. Compared with tape-based methods, this approach could also improve fit accuracy by capturing full shape and contour for required comfort, patient adherence, and therapeutic efficacy.
Studies show that adherence to prescribed self-care regimens among breast cancer survivors with BCRL is often suboptimal; in one cohort, only about 31 % of women maintained ≥ 75 % adherence to their self-care activities, indicating that the majority did not follow their complete treatment regimen as recommended. The primary barriers to consistent adherence include feelings of helplessness, a desire to feel “normal,” frustration from a lack of noticeable results, and inadequate support from social circles and healthcare professionals.
With visual 3D representations of body changes and their side-by-side comparisons over time, patients will be able to easily understand the progression of BCRL and treatment response, reinforcing adherence to prescribed therapies, supporting self-management, improving communication with care teams, and strengthening confidence in long-term treatment strategies. Last but not least, AI-powered 3D body-scanning technology could also help clinics and care teams generate standardized data to support documentation, communication, and coordinated decision-making.
Conclusion: The Future of BCRL Care
«An international team of researchers, led by Paula Donahue of Vanderbilt University Medical Center, wrote a paper highlighting how lymphedema’s long-term burden extends beyond considerable symptoms to significantly impact quality of life, psychosocial interactions, and emotional well-being. It also causes substantial financial burdens for patients, caregivers, payers, and society.»
Lia Colabello, Founder of Athena Aftercare
Integration of 3D body-scanning data into dedicated digital health platforms could empower both clinicians and patients by closing gaps in the symptoms, diagnosis and treatment of BCRL. Thus, AI-powered 3D body scanning may help shift BCRL management from an episodic and symptom-driven approach to a continuous and risk-based prevention.